Change management cited most frequently in survey
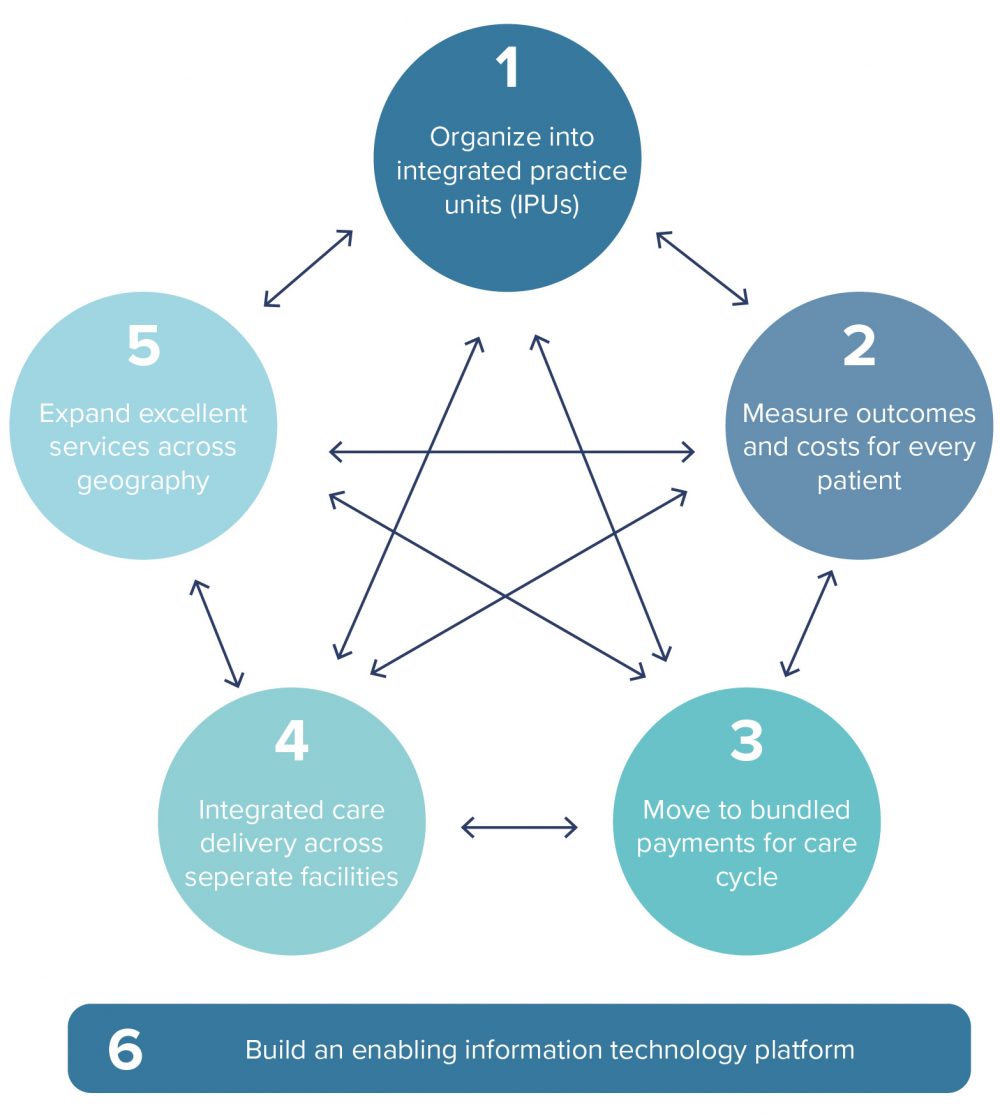
A Value-Based Healthcare (VBHC) market survey we recently conducted reveals that 41% of all hurdles cited which stand in the way of implementing VBHC are related to change management. The drawback of the VBHC Value Agenda created by Porter in 2013 (see figure 1) is that it only explains ‘what’ VBHC entails but not ‘how’ to actually achieve it, when in fact the process of implementing VBHC calls for fundamental change. This comes with its own set of challenges.
The three hurdles related to change management most frequently cited in the market survey include:
- Hurdle 1: There is both a lack of time and a lack of funds in order to be able to implement change (and no willingness to invest in doing so).
- Hurdle 2: Medical professionals fail to see the benefits for their own practice.
- Hurdle 3: The concept is too ambitious.
Change management is underestimated
It is a mistake to think you can accomplish change just like that, in addition to your day-to-day activities. This is certainly the case with a concept like VBHC, which basically involves a shift from controlling and organising healthcare volumes to managing and organising patient value. As this process challenges existing objectives, processes, structures and financial incentives, it requires nothing less than radical change.
The pitfall in this is that the content experts – usually the healthcare professionals themselves – also have to guide and lead the change. Regardless of the importance of input and enthusiasm in the workplace, the question is whether or not to make the healthcare provider responsible for the change process. It goes without saying that healthcare providers and professionals must be committed but, because they are already responsible for providing healthcare on a daily basis, you cannot expect them to simply take on this kind of major change in the course of their work. You can hardly ask someone to steer the boat while mending the sails at the same time.
Moreover, the change often has to occur using the available resources and budgets. Change takes time and energy and therefore requires additional resources, manpower and financial funds (Hurdle 1). Failure to turn the change process into an independent project ultimately results in delays and endless content-related discussions, without leading to real acceptance and actions. Defining, planning and budgeting for the change are essential steps.
Change management requires a structural approach
Change management is therefore a project in itself, one that requires a structural approach to the three key elements: mindset, culture and leadership.
1. Mindset
Implementing VBHC successfully means that improving patient value becomes the core of the day-to-day work, rather than something that is done on the side. VBHC is not the goal; instead, it is the means of improving patient value on an ongoing basis. Rather than being a standalone, isolated project, VBHC requires a change of mindset. It is a matter of using processes, work meetings and decision-making to improve patient value, and these aspects must be both experienced and felt (Hurdle 2).
2. Culture
Medical professionals are trained to make decisions and to act autonomously. Focusing on patient outcomes and making them transparent can be particularly daunting, as it directly affects the way medical professionals act. In addition, these professionals lose some of their autonomy. The process of implementing VBHC goes hand in hand with fostering a culture of improvement in which making ‘mistakes’ is all right provided we are open about it. It is all about seeing ‘mistakes’ as opportunities to learn and improve the quality and/or cost of healthcare. This requires a substantial shift in culture: from a culture that judges people to a safe culture of improvement, in which transparency is created for the purpose of improvement rather than punishment.
3. Leadership
Strong leadership is needed to accomplish cultural change: the hospital’s management board and the management of the specialist medical company must actively promote and practice VBHC. This includes supporting and promoting enthusiastic pioneers, rewarding good behaviour, embracing and promoting the culture of improvement mentioned above, and emphasising patient value in all communications. All key decisions must be made with the patient in mind. Patient value that is achieved on a long-term basis must be discussed and monitored in the boardroom on a regular basis.
Change management added to porter’s vbhc value agenda
In other words, change management must be an integral part of implementing VBHC, which is why we have expanded Porter’s VBHC Value Agenda by adding change management (see Figure 1). But we are not quite there yet, as VBHC remains a highly ambitious concept (hurdle 3). We can make VBHC more manageable by dividing it into pieces and placing it on a timeline, a topic which I will cover in a future blog post.