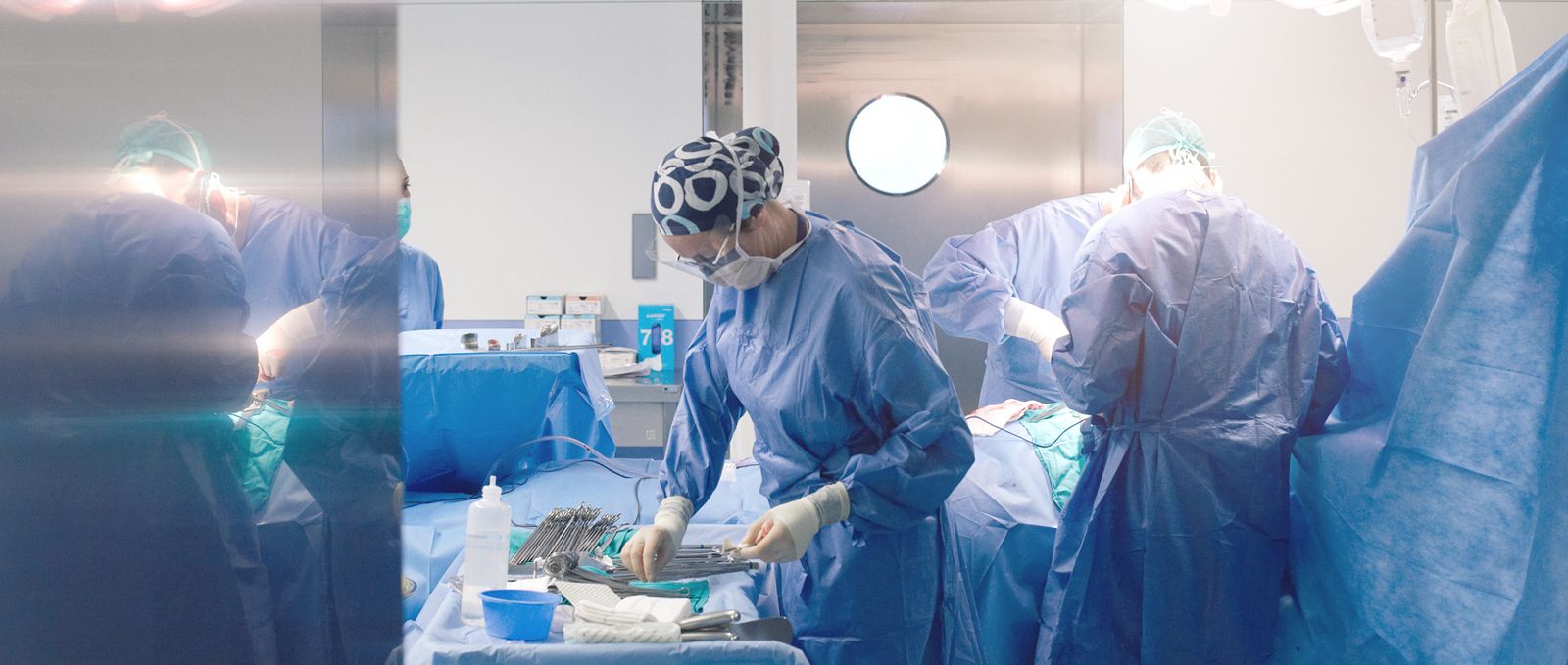
Almost every hospital is currently aware that there are great benefits to be gained from managing these ‘capacities’ in a more integrated way. These are benefits with respect to the quality of healthcare (shorter waiting times, faster throughput, more stable workload) and efficiency (efficient use of resources). But how to successfully get under way?
Forerunners lead the way
In the Netherlands, hospitals differ significantly in the extent to which they manage their capacity in an integrated way. Many hospitals have only recently started using this approach, and are still looking for the best way of kick-starting this transition. A few hospitals are already ahead of the rest. There are a number of interesting insights to be gained from looking at the approach taken by these forerunners.
Serious transition
To start with, it’s good to recognise that a proper transition is necessary for realising integrated capacity management, involving all levels of the hospital. ‘Integrated’ means that all departments coordinate their capacity together, with patient flow being the main priority. But it also means that there is an integrated flow from strategic objectives to operational capacity. These two movements will ideally be managed by a tactical planning body, which is a new kind of entity for many hospitals. In short: this is a major, hospital-wide change that requires serious attention.
Something that strikes me is that most hospitals have already been working for many years on improving their integrated capacity management, but with few real results to show for it yet. Frequently, they start out with a single capacity management project manager who first has to prove their worth before any further investment is made. This may sometimes work just fine for other new initiatives in hospitals, but it’s an inadequate approach for such a large task as this one. Outcomes are not realised, the hospital loses capacity, and the whole process feels like flogging a dead horse.
Phased approach or pressure cooker?
Which approach are the successful frontrunners using? I see roughly two types of transition taking place: the phased approach and what’s known as the ‘pressure cooker’ method.
The phased approach is a goal-oriented programme that spreads the transition over several years. This is only effective if the hospital starts out with a clear vision, goals and a step-by-step plan. The risk with this approach is that the organisation will postpone difficult transitions, so they have to wait a long time (too long) before seeing any successes.
A limited number of hospitals have used the ‘pressure cooker’ method. In this, the transition takes place over a relatively short period of time – one to two years at most. In addition to a clear vision from the Executive Board, this transition is often accompanied by extra urgency caused by another factor. Examples include relocation to new premises with significantly less capacity planned, or urgent financial problems. A familiar theme from change theory becomes clear in this case: that under pressure and at a certain speed, it’s possible to make changes that would otherwise take many years. This approach does have high costs in terms of investment in a project team with a number of people, and frequently also external support.
Both approaches are valid in themselves, and ensure that the hospital can realise the benefits of integrated capacity management over time. However, the preferred approach is the one in which external pressure causes the initiation of the transition; hospitals which have made use of this approach are now reaping the greatest benefits. The enablers are the same for all approach routes: a clear capacity management vision (Where are we going?), a case for change (Why is it necessary?) and a phased implementation plan with sufficient resources made available to achieve the desired goals. So, Board members, if you take capacity management seriously, choose the approach that best suits your organisation and your context, and give it the attention it deserves!