The meaning of Value in Value-Based Healthcare
In the first blog of our series, we have a special focus on the definition of value. The term Value-Based Healthcare is widely used by different healthcare stakeholders, however, value does not mean the same to all of them. In this blog we share the insights and key points highlighted by the World Economic Forum1,2,3, The European Expert Panel on effective ways of investing in Health (EXPH)4 from the European Commission, The Value of Health: Improving Outcomes (VoHIO) team5 and The Working Group6 regarding the definition of value.
The main driver: Sustainability
The need for change in healthcare systems is widely accepted and agreed upon. Costs are increasing faster than the available resources, making sustainability a big concern. All associations see aging and new technologies as a main driver for increasing costs. Additionally, wasteful spending is a common worry. The OECD has recently reported that up to 30% of healthcare spending is wasteful in part due to unnecessary/avoidable procedures.7 A new approach that values outcomes over volume is needed. Value-Based Healthcare has emerged as a way to focus healthcare efforts in bringing value to the patient. The importance of VBHC as an instrument of change is supported by the four associations unanimously. However, one of the main barriers recognized by most, is the lack of a common definition of Value.
Defining Value
In 2006, Professor Michael Porter and Professor Elisabeth Teisberg introduced the concept Value-Based Healthcare where value is defined as “health outcomes achieved per dollar spent”.8 The World Economic Forum follows Porter’s definition highlighting three fundamental principles of value-based care delivery. First, health outcomes that matter to patients should be measured systematically, ideally following global standards. Second, patient groups should be segmented according to patient condition and risk level. Finally, segment specific interventions should be implemented to improve the value of each sub-group.
Over the years, more comprehensive definitions of Value have emerged in the European context. These new definitions bring additional value components. In total, 5 dimensions are recognized: Personal, Technical, Population (or Allocative), Societal and Macroeconomic.
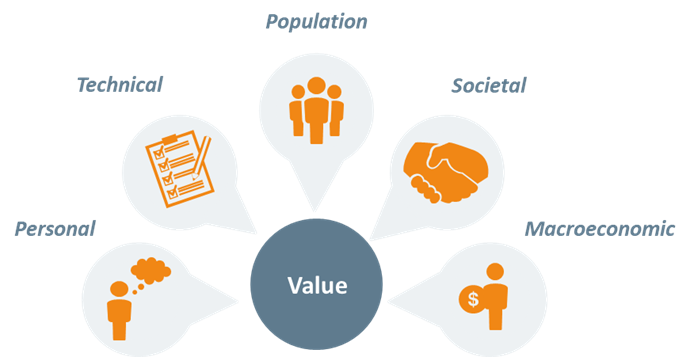

The Personal, Technical and Population Value components were introduced by Prof. Gray and colleagues in 2017 in their Triple Value Model.9 Personal value refers to improving outcomes that matter to each individual patient, recognizing the importance of patient’s experience in healthcare and shared decision making. Technical value refers to the optimization of care to achieve maximum outcomes with a given amount of resources. Population value refers to allocating and investing resources wisely at the population level to optimize healthcare and wellbeing of the whole population.
In 2019, the EXPH included the Societal value component, which refers to whether the healthcare intervention has an impact on social aspects such as social cohesion, solidarity, mutual respect, equity, etc.4 The Societal value is not a set of tools, but rather a perspective that should be considered when looking at Value. It also implies looking at outcomes and costs for the patient and caregivers that go beyond health outcomes. For example, the costs related to the loss of productivity of both patient and carers, as pointed out by the Working Group.6
Finally, the Macroeconomic perspective is mentioned by the Working Group and looks at the value of statistical life.6 Going beyond the value of productivity loss it looks at the value of living longer and healthier lives. For example, added economic value is expected as people expect to live longer and invest in their children and pension, further driving economic growth.
In the following table, we compile the various value components presented by the different organizations and indicate the focus of each of them as presented recently in their respective reports.
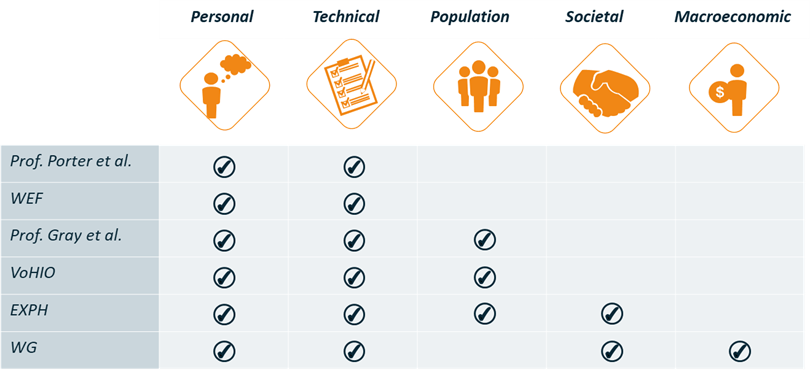

Defining value at the EU level
As follows from the previous definitions and table 1, it is clear that European organizations strive for a more comprehensive definition of value that goes beyond Porter’s. The initial definition presented by Porter, is closely related to the Technical value and incorporates Personal value components as presented by the EXPH. This definition is not comprehensive enough for countries striving for Universal Health Coverage (UHC), where there is a commitment to fulfill the healthcare needs of the whole population. For the European associations two key values need to be incorporated in the definitions: Solidarity and Equity. These values are at the core of the European society and should therefore be considered when defining value in the Healthcare context.
We hope you enjoyed this blog, in the next blog, we will focus on some practical aspects of VBHC implementation and discuss the recommendations from international and European organization to get ready for the transition.




